LRS
2022-03-30 2022-03-30 14:57LRS
Abstract
Background:
Management of open tibial diaphyseal fractures with bone loss is a matter of debate. The treatment options range from external fixators, nailing, ring fixators or grafting with or without plastic reconstruction. All the procedures have their own set of complications, like acute docking problems, shortening, difficulty in soft tissue management, chronic infection, increased morbidity, multiple surgeries, longer hospital stay, mal union, nonunion and higher patient dissatisfaction. We evaluated the outcome of the limb reconstruction system (LRS) in the treatment of open fractures of tibial diaphysis with bone loss as a definative mode of treatment to achieve union, as well as limb lengthening, simultaneously.
Materials and Methods:
Thirty open fractures of tibial diaphysis with bone loss of at least 4 cm or more with a mean age 32.5 years were treated by using the LRS after debridement. Distraction osteogenesis at rate of 1 mm/day was done away from the fracture site to maintain the limb length. On the approximation of fracture ends, the dynamized LRS was left for further 15-20 weeks and patient was mobilized with weight bearing to achieve union. Functional assessment was done by Association for the Study and Application of the Methods of Illizarov (ASAMI) criteria.
Results:
Mean followup period was 15 months. The mean bone loss was 5.5 cm (range 4-9 cm). The mean duration of bone transport was 13 weeks (range 8-30 weeks) with a mean time for LRS in place was 44 weeks (range 24-51 weeks). The mean implant index was 56.4 days/cm. Mean union time was 52 weeks (range 31-60 weeks) with mean union index of 74.5 days/cm. Bony results as per the ASAMI scoring were excellent in 76% (19/25), good in 12% (3/25) and fair in 4% (1/25) with union in all except 2 patients, which showed poor results (8%) with only 2 patients having leg length discrepancy more than 2.5 cm. Functional results were excellent in 84% (21/25), good in 8% (2/25), fair in 8% (2/25). Pin tract infection was seen in 5 cases, out of which 4 being superficial, which healed to dressings and antibiotics. One patient had a deep infection which required frame removal.
Conclusion:
Limb reconstruction system proved to be an effective modality of treatment in cases of open fractures of the tibia with bone loss as definite modality of treatment for damage control as well as for achieving union and lengthening, simultaneously, with the advantage of early union with attainment of limb length, simple surgical technique, minimal invasive, high patient compliance, easy wound management, lesser hospitalization and the lower rate of complications like infection, deformity or shortening.
Keywords: Bone loss, fracture tibia, limb reconstruction system
MeSH terms: Tibial fracture, fractures, compound, reconstructive surgical procedure
Introduction
Tibia being a subcutaneous bone, open fractures of the tibia with massive soft tissue injury and bone loss, has become a problem for all trauma surgeons.1 The specific method of treatment of these fractures is a matter of debate, with the treatment options ranging from external fixators, ring fixators, nailing, plating, tibial synostosis, free or vascularized bone grafting along with allografts or bone substitutes, all having their own set of complications.1,2,3,4 Ring fixators have given the best results in these fractures but are cumbersome both for the patient as well as the surgeon5,6,7,8,9 and are technically demanding procedures. The limb reconstruction system (LRS) consists of an assembly of clamps (usually two or three) which can slide on a rigid rail and can be connected by compression-distraction units to achieve bone transport. In this prospective study, we evaluated the outcome of the LRS in the treatment of open fractures of tibial diaphysis with bone loss as a definite mode of treatment to achieve union, as well as limb lengthening, simultaneously.
Materials and Methods
Thirty prospective cases of open fractures of tibial diaphysis with bone loss treated by using the LRS to achieve union and lengthening simultaneously between 2009 and 2012 constituted the study.
The inclusion criteria were patients between 20 and 55 years, Gustilo Anderson type III A and III B with injury severity score10 of at least 5 and bone loss of 4 cm or more. Closed fracture, infected gap nonunion, osteoporotic fracture, followup less than one year or metaphyseal fractures were excluded from the study. Clearance from the institutional ethical committee was taken.
Initially, primary survey done to diagnose associated injuries and prevent life threatening complications. After advanced trauma life support resuscitation, thorough irrigation of the wound and primary splintage with crammer wire done. Third generation intravenous cephalosporin was given. Preoperative workup involved taking X-rays of the entire affected leg with knee and ankle – anteroposterior (AP) and lateral views
Operative procedure
All patients were taken for immediate surgical debridement with removal of all dead necrotic tissues, removing the free loose bone pieces, followed by stabilization of the fracture with application of LRS system, under spinal anesthesia under a tourniquet and image intensifier in the supine position. Tourniquet was inflated only after the debridement was completed and before osteotomy.
Schanz pins of LRS were inserted by longitudinal stab incision and separating the soft tissue down to the bone by blunt dissection on the anteriomedial surface of tibia hence preventing the risk of neurological, vascular or tendon injuries. First the proximal most, Schanz screw was inserted by sequentially predrilling with an appropriate-size bit, followed by manual insertion of the Schanz screw by the T handle, which lowers the risk of thermal necrosis and pin loosening. This proximal pin was placed at least 15 mm from the joint to avoid penetration of the joint capsule and avoid the pes tendons and patellar tendon. Then the distal most, Schanz screw inserted in the same manner. The rod and assembly connected over these proximal and distal pins maintaining the leg length and this definitive fixator was used as a guide to pass the rest of the pins, to ensure that the rail is parallel to the long axis of the bone and all the remaining screws will be on the bone, in the same plane, perpendicular to the long axis of the tibia and parallel to the knee and ankle joints and aligning the tibial tuberosity with the second metatarsal. The foot and ankle were manipulated to ensure the absence of musculotendinous tethering. We used three Schanz screws each in the proximal and distal end clamps respectively and two screws in the middle mobile clamp. All Schanz screw were inserted under C arm control so that not more than about 2 mm was protruding beyond the distal cortex, as trying to back them out can cause pin loosening because of the tapering design of pins. After putting all the pins and the fixator on the limb, the pin holding nuts (clamps) were tightened. The compression-distraction unit was put on the proximal end clamp and middle clamp in the holes provided. Low energy osteotomy was done between the proximal and middle clamps using either a gigli wire or with a thin osteotomy connecting the predrilled holes. Through two incisions anteriorly and posteromedially periosteum was elevated, and a gigli saw was passed over a tape gauze subperiosteally from posteriomedial to anterior incision. With the gigli saw the bone was cut till it reached the medial cortex and then by periosteum elevator passed subperiosteally the osteotomy completed, protecting the periosteum. In none of the case, acute docking attempted. After thorough lavage and sterile dressing, the wound was left open without trying the wound coverage methods.
Postoperatively systemic antibiotic were continued for 5 days and dressing done regularly. In patients, whose bone was exposed, as the wound condition improved the patients were planned for flap rotation. In the rest of the patients, the wound was left as such to heal, with secondary intention or if required, split skin grafting was done. Distraction of the osteotomy was started after a week of the osteotomy at the rate of one fourth turn 4 times a day resulting in a total bone transport of 1 mm/day or 7 mm/week. In some patients rate of distraction was altered during the distraction phase depending on the patient compliance and the type of regenerate. Patients were encouraged to attain knee and ankle range of motion (ROM) after the application of LRS, depending on the patient pain tolerance.
This bone transport was continued till the fracture end approximated. And when the bone ends approximated, the distraction was stopped and dynamization of the LRS system done, which was followed by weight bearing mobilization by the patient as per his tolerance [Figures [Figures11 and and2].2]. The dynamized LRS system was left in situ for further 15-20 weeks for consolidation of the regenerate and fracture union to occur. After the union and consolidation phase that is, till the three cortex union seen on the AP and lateral views, the LRS system was removed and the patellar tendon bearing cast was applied allowing full weight bearing, for further 6-10 weeks. Since the LRS remained for a period of about a total of 24-50 weeks, by this time in all cases the regenerate was well consolidated. Bony and functional assessment was done by Association for the Study and Application of the Methods of Illizarov (ASAMI) criteria,11 based on union, infection, limb length discrepancy and deformity at the docking site and patient activity, limping, stiffness, reflex sympathetic dystrophy and pain, respectively.

Immediate postoperative anterior-posterior (AP) (a) and lateral (b) view of a 35-year-old male presenting with open grade III B fracture tibia right side with 5 cm bone loss after debridement, application of limb reconstruction system (LRS) and osteotomy with three pins in proximal and distal fragments respectively and two pins in middle mobile fragment. 10 weeks followup AP (c) and lateral (d) of the patient after distraction showing approximation of the bone ends and regenerate. 28 weeks postoperative AP (e) and lateral (f) view after consolidation phase of 18 weeks with dynamized LRS showing three cortex union. 35 weeks postoperative AP (g) and lateral (h) view and clinical photographs (i and j) of a limb after patella tendon bearing cast removal showing good alignment of the limb with healing of the wound and knee range of motion
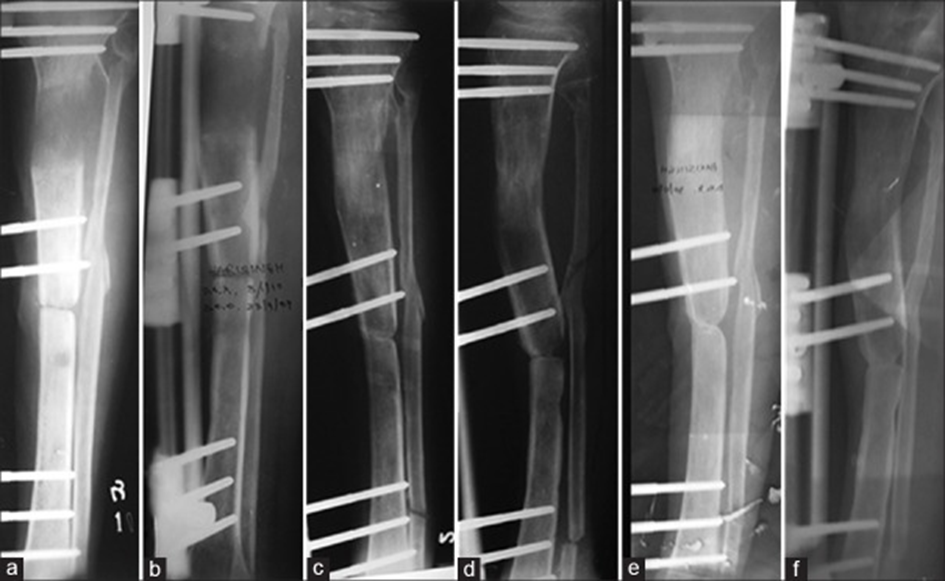
Followup X-rays anterior-posterior (AP) (a) and lateral (b) view of a 40 years old male with open tibial fracture with 6 cm bone loss, 12 weeks of distraction after application of limb reconstruction system (LRS) showing approximation of the bone ends and regenerate. 30 weeks postoperative AP (c) and lateral (d) view after consolidation phase of 18 weeks with dynamized LRS. 35 weeks postoperative AP (e) and lateral (f) view after the end of consolidation phases showing adequate union, regenerate and alignment
Results
The results are assessed in 25 patients. 5 patients were lost to followup and hence excluded from the study. Mean age of the patients was 32.5 years (range 20-48 years). 92% (n = 23) patients were males with road traffic accident (92%) as the major cause of injury while rest (n = 2) sustained injury due to fall from height. 92% (n = 23) of the fractures were located in the middle or lower third of the tibia. Mean followup period was 15 months (range 12-19 months). Wound healed completely itself (n = 20) along with distraction – histogensis probably because of increased vascularity at the fracture site with distraction, whereas, additional skin grafting was done in 3 and fasciocutaneous flap rotation done in 2 cases only within one week as the wound condition improved.
The mean bone loss was 5.5 cm (range 4-9 cm). The mean duration of bone transport to fill this gap that is, time from application of LRS till the bones approximated after distraction, was 13 weeks (range 8-30 weeks). The mean time for LRS in place was 44 weeks (range 24-51 weeks), this is the time from application of LRS till its removal, which includes time of 1-week waiting, distraction or bone transport time to fill bone gap of 4-9 cm and 15-20 weeks time for fracture consolidation. The mean implant index was 56.4 days/cm. After three cortex union seen on AP and lateral view, removal of the LRS done and the patella tendon bearing (PTB) cast was further given for 6-10 weeks for union to consolidate and pin tracts to heal. Thus mean time to union that is, from application of LRS till removal of PTB cast was 52 weeks (range 31-60 weeks) with mean union index of 74.5 days/cm [Figures [Figures1,1, ,22 and Table 1].
Table 1
Results of LRS in open tibial fractures with bone loss
Bony results as per ASAMI score were excellent in 76% (n = 19), good in 12% (n = 3), fair in 4% (n = 1) and poor in 8% (n = 2). Functional results were excellent in 84% (n = 21), good in 8% (n = 2), fair in 8% (n = 2). Poor and failure was seen in none of our patients [Table 2]. Union occurred on dynamized LRS and PTB cast in all except 2 (8%) patients who developed nonunion at docking site and had poor results and required additional bone grafting and plating to achieve union. In one patient the LRS was removed earlier due to infection whereas in other the LRS was used for an extended period, but it failed to show three cortex union on LRS and hence operated for grafting and plating. At final followup leg length discrepancy of more than 2.5 cm was found in only 2 (8%) cases, rest 23 (92%) having leg length discrepancy of <2.5 cm and were able to walk without shoe raise. None of the patient had deformity more than 7° The knee ROM, at final followup was more than 120° in 84% (n = 21) cases and ankle ROM of more than 30° in 92% (n = 23) case. The most common complication encountered was pin tract infection in 5 cases, out of which 4 being superficial which healed to dressings and antibiotics. 1 patient had a deep infection which required frame removal and subsequent debridement and finally on healing of infection, the nonunion, required plating and bone grafting [Figure 3]. Aseptic pin loosening occurred in 2 cases and was managed by further advancing the tapering pins. 1 patient developed skin reaction after fixator application and had to be put on steroids and antiallergic medication for 5 days. There were no cases of neurovascular compromise, joint subluxation or refracture.
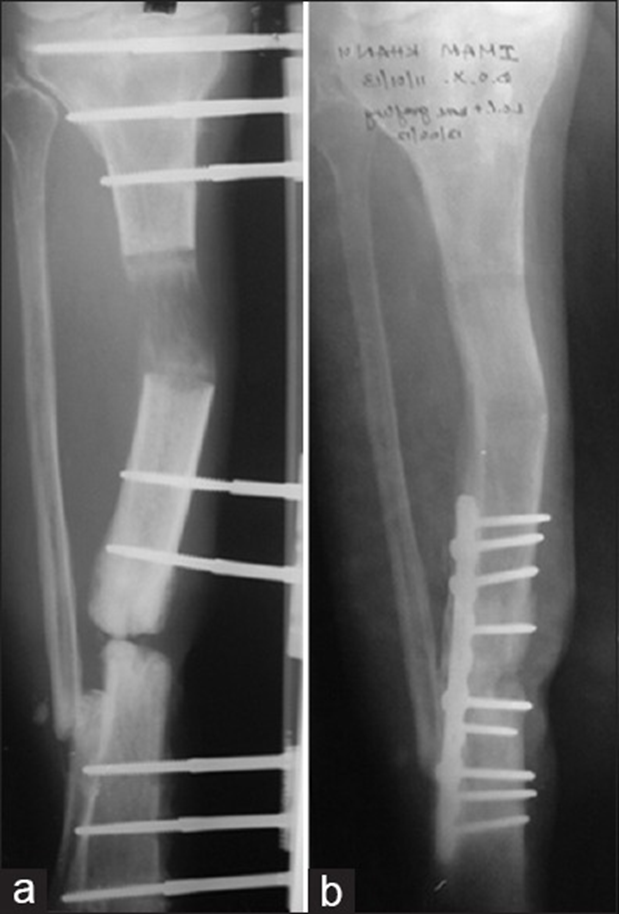
Postoperative anteroposterior (AP) (a) of a patient with open grade III B fracture tibia right side with 7 cm bone loss, after 3 months application of limb reconstruction system (LRS) showing infection and nonunion. The patient underwent removal of LRS and subsequent debridement and after healing of the wound successfully treated with plate and bone-grafting AP (b) view
Table 2
Bony and functional results as per ASAMI criteria



